Parkinson's disease: practical guide to symptoms, treatment, and daily life
Parkinson's disease is a movement disorder that affects about 1% of people over 60. It starts slowly and shows up differently in everyone. If you or someone you care for has new tremor, stiffness, slowness, or balance trouble, this page gives clear, usable steps to recognize symptoms, find the right care, and make daily life safer.
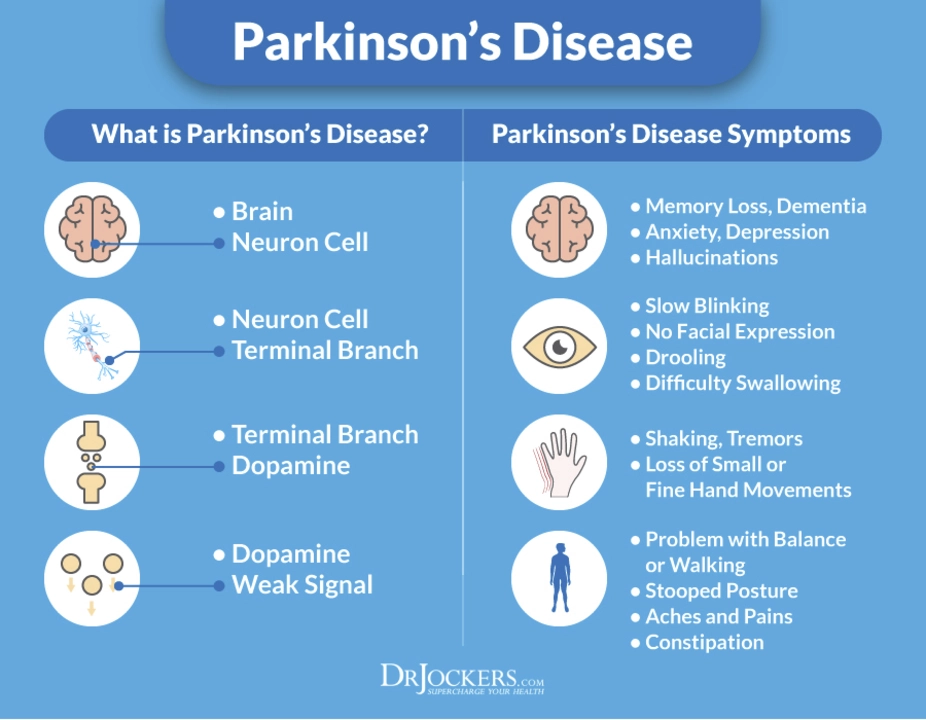
Recognize the signs and get a timely diagnosis
Early signs can be subtle: a slight tremor in one hand at rest, one-sided stiffness, a slower walk, or softer voice. Mood changes, constipation, and poor sleep often appear years before movement problems. If you notice a pattern, see a family doctor or a neurologist who treats movement disorders. Bring a short video of symptoms and a list of medicines — that helps speed diagnosis. Doctors use clinical exams and sometimes imaging to rule out other causes.
Treatment options that actually help
Levodopa is the most effective drug for controlling motor symptoms. It turns into dopamine in the brain and improves walking, stiffness, and tremor. Dopamine agonists (like pramipexole) and MAO-B inhibitors (like rasagiline) are other options, often used earlier or alongside levodopa. For wearing-off or dyskinesia, strategies include adjusting dose timing, adding COMT inhibitors, or switching to advanced therapies such as deep brain stimulation (DBS) or continuous delivery systems.
Small clinical trials have also tested diabetes drugs called GLP-1 agonists (for example, exenatide) and reported slowed motor decline over a year in some patients. That’s promising, but these options are still being studied and aren’t standard care yet. Always discuss risks, benefits, and monitoring with your neurologist before trying new or off-label treatments.
Non-drug therapies make a big difference. Regular exercise—especially boxing-style training, tai chi, or balance work—helps mobility and reduces falls. Speech therapy can improve volume and swallowing. Occupational therapy teaches energy-saving techniques and safe ways to handle daily tasks.
Safety matters: Parkinson's increases fall risk and can cause low blood pressure when standing. Keep floors clear, use night lights, consider grab bars, and discuss home safety with an occupational therapist. Keep a medication log and wear a medical ID if you have advanced disease or take multiple drugs that cause drowsiness.
Practical tips: schedule meds around activities you need most, set phone alarms for doses, and track 'on' and 'off' times to share with your doctor. For digestion issues, spread fluids and fiber through the day and talk to your care team about constipation remedies.
Find support: look for a movement disorder clinic, Parkinson's support groups, and trusted online resources. Ask for referrals to physiotherapy and speech therapy early—those services pay off fast.
If you notice new tremor, slower movement, or balance problems, make an appointment now. Early treatment and practical changes improve quality of life and keep you moving longer.
Amiloride and its potential use in the treatment of Parkinson's disease
I recently came across some fascinating research on Amiloride, a diuretic drug, and its potential use in the treatment of Parkinson's disease. Studies have shown that Amiloride may help slow down the progression of this debilitating condition by protecting dopamine-producing neurons. This is a significant breakthrough, as it could potentially improve the quality of life for millions of people affected by Parkinson's. While more research is needed to fully understand its effects, I'm optimistic that Amiloride could become a valuable tool in the fight against Parkinson's disease. Stay tuned for more updates on this exciting development!