Patient care: simple, practical steps to stay safer with meds
About half of people with long-term conditions miss doses or use medications wrong. That matters because small mistakes — wrong timing, mixing drugs, or bad storage — can cause side effects, worse health, or extra trips to the ER. This page gives short, usable steps you can apply today to make medication and home care safer for you or someone you look after.
Manage meds like a pro
Keep a single, up-to-date list of every medication, dose, and why you take it. Put it on paper and on your phone. Show that list at every doctor visit and when you order from an online pharmacy. Use a weekly pillbox or daily blister packs and set alarms on your phone — simple reminders cut missed doses a lot.
When starting a new drug, write down two things: what to expect and what side effects need a call to your clinician. For example, some antidepressants can cause sleep changes or appetite shifts in the first weeks. If you notice sudden breathing trouble, high fever, severe rash, fainting, or chest pain, get urgent care.
Safe ordering, storage, and switching
If you buy meds online, pick a verified pharmacy, keep records of prescriptions and receipts, and confirm the active ingredient matches your prescription. For Canadians, check pharmacy licensing or trusted review lists before ordering. Avoid sites that skip prescriptions for prescription-only drugs.
Store meds where they stay dry and at recommended temperatures — most go in a cool, dry place, not the bathroom. For insulin or biologics, follow fridge rules exactly. Throw out expired medicine; don’t flush it. Many pharmacies offer take-back bins for safe disposal.
Switching brands or generics can change how a medication feels. If your blood pressure or blood sugar spikes after a switch, measure at home and contact your prescriber — don’t stop the medicine without advice. Ask your pharmacist how to compare generics and whether monitoring is needed after a change.
Keep regular lab tests if your drug needs monitoring. For example, anticoagulants, some antipsychotics, and diabetes meds often require blood work. Set calendar reminders and stick to the schedule — labs catch problems early.
Caregivers: use clear labeling and short instructions. Mark morning and night doses with colored stickers. Teach the person you care for what each pill is for in one sentence — repetition helps. If you handle multiple people’s meds, separate storage areas to avoid mix-ups.
Finally, communicate. Tell your clinician about herbal supplements, over-the-counter drugs, and alcohol — these commonly interact with prescriptions. Ask one clear question each visit: “Is this medicine still best for me?” Small questions prevent big problems and keep care practical and safe.
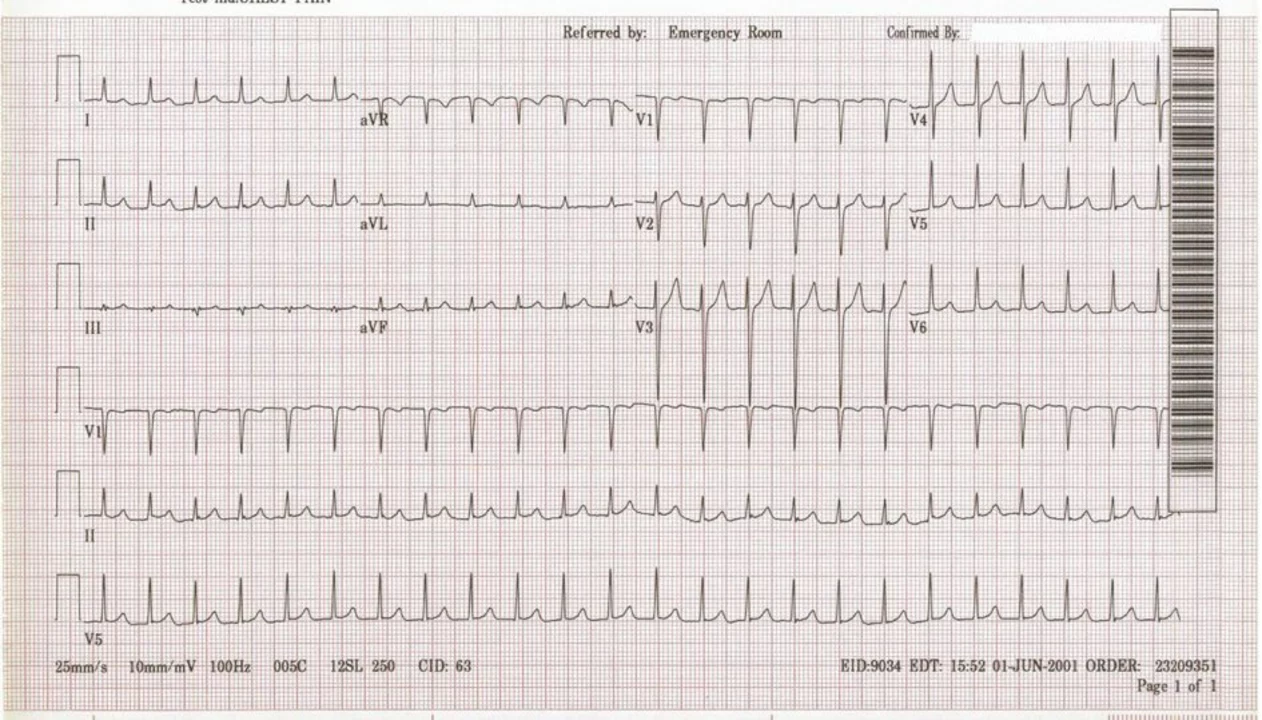
The Importance of Regular Check-ups for Supraventricular Tachycardia Patients
As a supraventricular tachycardia (SVT) patient, I cannot stress enough the importance of regular check-ups. Staying on top of my health and monitoring my heart's condition helps me manage my symptoms and prevent complications. With regular doctor visits, I can also receive tailored advice and adjust my treatment plan if necessary. Additionally, these check-ups give me peace of mind and let me lead a more active lifestyle without constant worry. So, if you're an SVT patient like me, make sure to prioritize your regular check-ups for a healthier and happier life.