Ocular Hypertension: What High Eye Pressure Means for Your Vision
Noticed “high pressure” in your eye exam but your doctor says your optic nerve looks fine? That’s ocular hypertension — elevated intraocular pressure (IOP) without detectable glaucoma damage. It’s not an emergency, but it’s not something to ignore either. Knowing how it’s checked, what raises your risk, and what you can do every day helps keep your vision safe.
How it’s diagnosed
IOP is measured in millimeters of mercury (mmHg). Most doctors consider pressure above about 21 mmHg to be higher than normal, but numbers are only part of the story. Your eye doctor will also look at the optic nerve with ophthalmoscopy or OCT imaging and test your visual field to check for early signs of glaucoma.
Other things that affect interpretation: corneal thickness (a thin cornea can make pressure look lower than it is), family history of glaucoma, age, and past eye injuries. If any risk factors are present, your doctor may recommend closer monitoring or early treatment.
Treatment and daily tips
Treatment aims to lower IOP to reduce the chance of developing glaucoma. First-line options are medicated eye drops: prostaglandin analogs, beta-blockers, carbonic anhydrase inhibitors, and alpha agonists. Your doctor will choose based on how high your pressure is, your other medical conditions, and possible side effects.
Laser therapy (selective laser trabeculoplasty) is a common next step if drops aren’t enough or you’d prefer fewer daily meds. Surgery is reserved for stubborn cases where other options don’t control pressure.
Practical tips that help right now:
- Take eye drops exactly as prescribed and at the same time each day. Missing doses reduces effectiveness fast.
- Learn punctal occlusion: press the corner of your eye for one minute after a drop to lower systemic absorption and side effects.
- Keep follow-up visits. IOP can change slowly — only regular tests catch that early.
- Talk about costs and generics if insurance is tight; many effective generics are available.
- Avoid head-down yoga poses and heavy Valsalva (straining) if your doctor warns you — these can raise IOP temporarily.
Other lifestyle moves matter too: regular exercise (moderate cardio) can lower eye pressure for many people, and smoking worsens overall eye and vascular health. High caffeine intake may give a temporary IOP spike in some people, so watch how your body reacts.
When to call your doctor: sudden eye pain, blurred vision, halos around lights, or a dramatic change in vision need immediate attention. For routine changes in pressure or side effects from drops, schedule a prompt clinic visit so treatment can be adjusted before damage occurs.
Ocular hypertension isn’t a sentence — it’s a signal. With the right tests, sensible monitoring, and practical day-to-day habits, you can lower your risk and protect your optic nerve. Ask your eye doctor for a clear plan: target IOP, testing schedule, and what signs you should watch for at home.
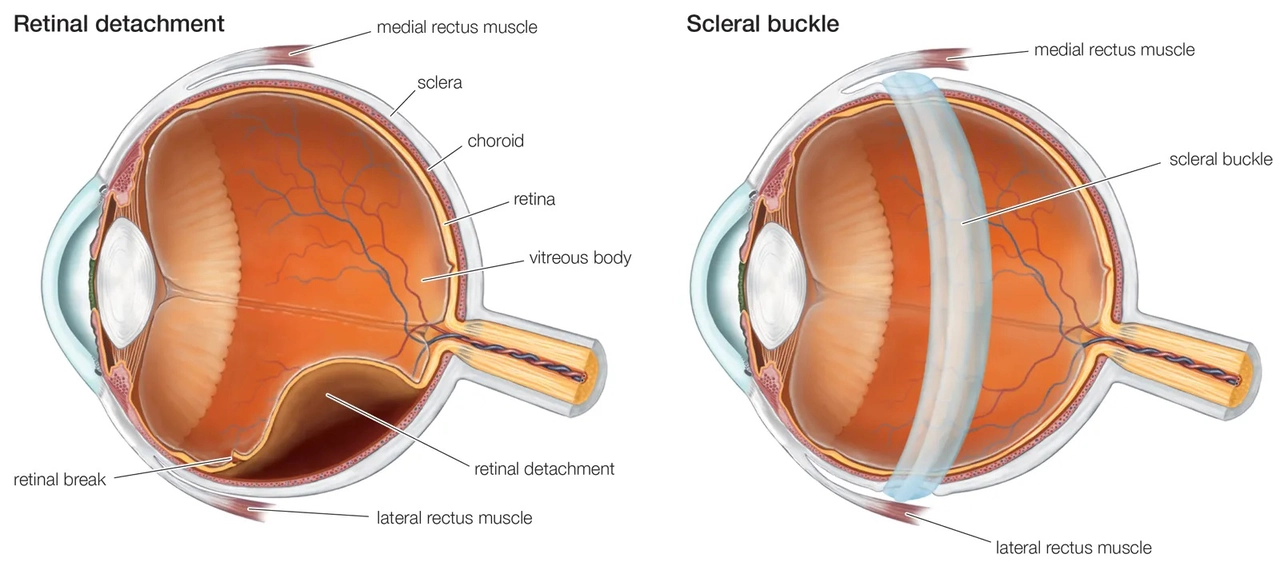
The Relationship between Ocular Hypertension and Retinal Detachment
In a recent study, I came across the fascinating connection between ocular hypertension and retinal detachment. Ocular hypertension, characterized by increased pressure within the eye, has been found to potentially contribute to retinal detachment, a serious condition where the retina pulls away from its supporting layers. This relationship is crucial to understand, as early detection and management of ocular hypertension can help prevent the development of retinal detachment. Moreover, retina specialists should be aware of this correlation to ensure they provide the best care for their patients. Overall, understanding the link between these two eye conditions can lead to improved eye health and vision preservation.