Retinal detachment: how to spot it and what to do now
A retinal detachment can steal your vision quickly. If you see a sudden shower of floaters, flashes of light, or a dark curtain over part of your sight, treat it like an emergency. Acting fast gives the best chance to save vision.
Signs and first steps
Watch for these clear warning signs: a sudden increase in tiny floating specks, brief flashes of light, a shadow or curtain moving across your field of view, or a sudden drop in sharpness. These symptoms can start in one eye and get worse over hours or days.
If you notice any of these, call your eye doctor or go to the emergency department right away. Don’t wait for a scheduled appointment. Until you can see a specialist, avoid heavy lifting, intense exercise, and rubbing your eyes.
How doctors check and what to expect
An eye specialist will dilate your pupil and examine the retina with special lenses. If the view is blocked by blood or swelling, they may use an ocular ultrasound. Tests are fast and usually painless.
Treatment depends on the type and size of the detachment. If the retina has a small tear but hasn’t fully detached, outpatient methods like laser (photocoagulation) or freezing (cryopexy) can seal the hole. If the retina has pulled away, surgery is often needed.
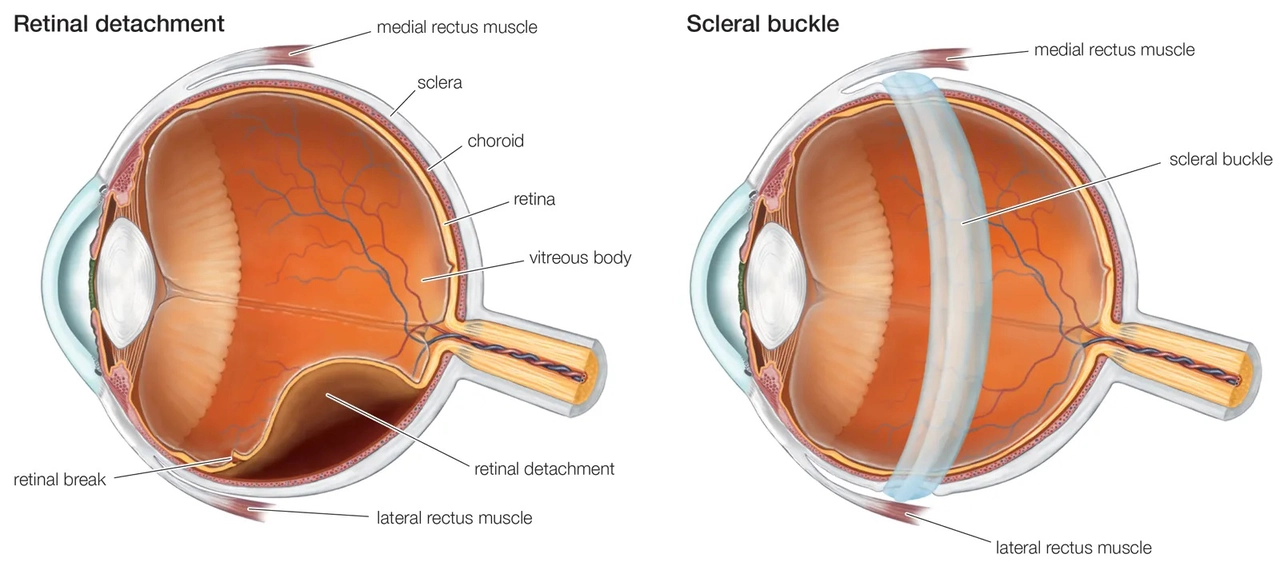
Surgical options include pneumatic retinopexy (a gas bubble is placed to push the retina back), scleral buckle (a silicone band supports the eye from the outside), and vitrectomy (removal of vitreous gel and reattachment of the retina). Your surgeon will explain which fits your situation and the trade-offs: speed of recovery, success rates, and activity limits after surgery.
Recovery varies. You may need to keep your head in a certain position for days if a gas bubble was used. Vision can improve over weeks to months, but final clarity depends on how long the retina was detached and whether the central retina (macula) was involved. Some permanent vision loss can occur, especially if treatment is delayed.
Follow-up care matters: frequent checks after surgery catch problems early. Your doctor may advise avoiding air travel while a gas bubble is present and will give clear timelines for returning to normal activities.
Preventive steps help those at higher risk: get regular eye exams if you’re very nearsighted, have a family history of retinal detachment, or had eye surgery or trauma. Wear eye protection during sports and report any new flashes or floaters right away.
Don’t ignore sudden changes in vision. Quick action—calling your eye doctor or heading to the ER—gives you the best shot at keeping good sight.
The Relationship between Ocular Hypertension and Retinal Detachment
In a recent study, I came across the fascinating connection between ocular hypertension and retinal detachment. Ocular hypertension, characterized by increased pressure within the eye, has been found to potentially contribute to retinal detachment, a serious condition where the retina pulls away from its supporting layers. This relationship is crucial to understand, as early detection and management of ocular hypertension can help prevent the development of retinal detachment. Moreover, retina specialists should be aware of this correlation to ensure they provide the best care for their patients. Overall, understanding the link between these two eye conditions can lead to improved eye health and vision preservation.